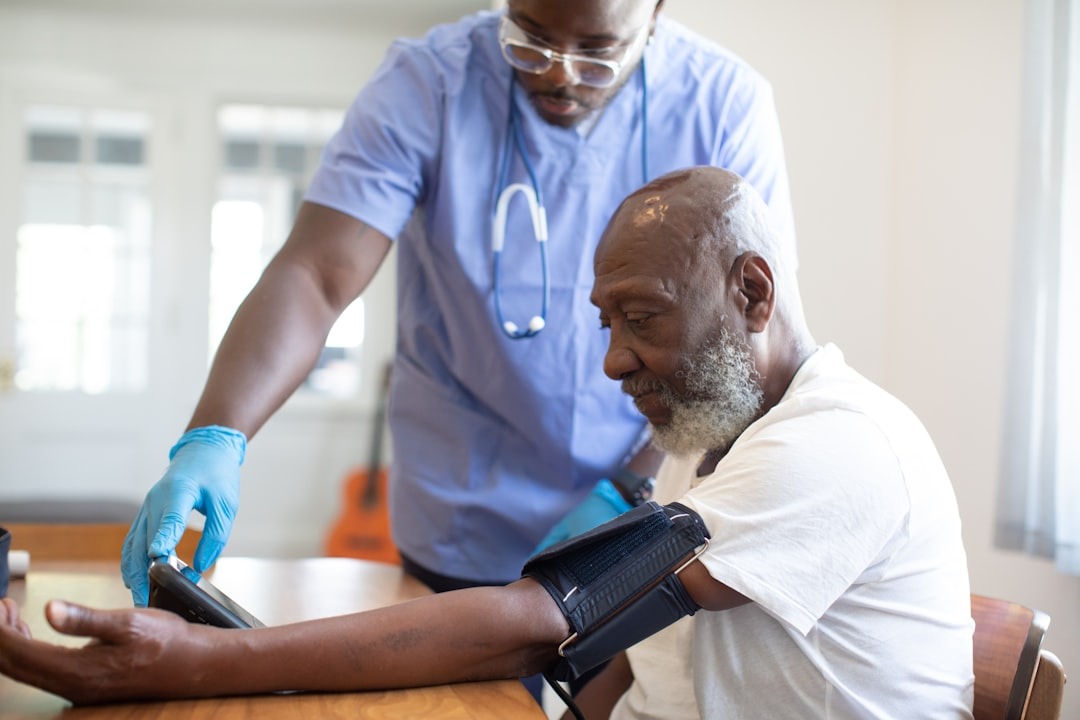
Medicare Advantage Plans Explained: Your Essential Guide
March 2, 2026
Understanding Medicare Advantage Plans: A Guide
As your 65th birthday approaches, your mailbox likely overflows with flyers promising the “best” Medicare plan. This wave of information can be confusing, but understanding one key choice can make it all clear for healthcare planning. Recent headlines about a Medicare Advantage marketing rule judge decision highlight why it’s wise to rely on official, unbiased resources when comparing options. That choice is whether to stick with Original Medicare or select a Medicare Advantage plan.
A Medicare Advantage plan is an alternative path—not a supplement—to receiving your benefits. These are the Medicare Advantage plans you often see advertised with $0 premiums and extra perks, offered by private insurance companies approved by Medicare. Making sense of this option is the first step toward confident decision-making. This guide breaks down what Medicare Advantage is, how the plans work, and the real-world trade-offs between lower costs and network rules.
Path 1 vs. Path 2: How ‘Original Medicare’ and ‘Advantage Plans’ Differ
When you enroll in Medicare, you face a foundational choice in how to receive your benefits. You can either use the traditional government-run program or choose an all-in-one plan from a private insurer. This decision sets the stage for how you’ll access and pay for your healthcare.
Original Medicare is à la carte—you get hospital (Part A) and medical (Part B) coverage from the government and can add separate drug coverage (Part D).
In contrast, a Medicare Advantage (Part C) plan is a bundled combo meal. Private companies offer these plans, combining Parts A, B, and usually D into one package, often with extras like dental and vision.
Two main paths to Medicare coverage
When you enroll in Medicare, you’ll typically choose between Original Medicare or a Medicare Advantage plan. Here’s a quick side-by-side:
| Feature | Original Medicare (Path 1) | Medicare Advantage (Path 2) |
| How you get it | Provided through the federal government | Offered by private insurers approved by Medicare |
| What it covers | Part A (hospital) + Part B (medical) | Covers all Part A + Part B services |
| Extra benefits | Typically not included | Often includes dental, vision, hearing, and fitness perks |
| Prescription drugs | Requires a separate Part D plan | Commonly included within the plan |
| Provider choice | You can generally see any provider nationwide that accepts Medicare | You’ll usually use providers within the plan’s network |
The main trade-off is freedom versus structure. Original Medicare offers flexibility to see almost any doctor, but your out-of-pocket costs can be unpredictable without a separate Medigap supplement policy. Medicare Advantage plans provide predictable costs and extra perks, but usually require you to stay within a network of providers.
How Do Medicare Advantage Plans Actually Work?
Choosing a Medicare Advantage plan means you’re asking a private insurance company to manage your healthcare benefits on behalf of the government. These companies operate under a strict contract with Medicare and are required by law to provide, at a minimum, all the same hospital (Part A) and medical (Part B) coverage that Original Medicare provides. This ensures you receive the core benefits you’re entitled to, just delivered through a different system. Private insurers such as Humana Medicare Advantage and many others administer these plans under federal rules and oversight.
You’ve probably seen commercials for Advantage plans with a $0 monthly premium. While many such plans exist, you must still pay your monthly Part B premium to the government. Think of the Part B premium as your membership fee for the entire Medicare system. Once enrolled in an Advantage plan, your new plan ID card becomes your primary insurance card for doctors and hospitals, not your red, white, and blue Medicare card.
Getting More Than the Basics: Dental, Vision, and Other Perks
Original Medicare (Parts A and B) doesn’t cover routine dental care, eye exams for glasses, or hearing aids. Medicare Advantage plans create a compelling alternative by filling these gaps, often bundling dental, vision, and hearing benefits into a single policy. For many, this is simpler and more affordable than purchasing separate coverage.
Beyond eyes and teeth, the vast majority of Advantage plans also include prescription drug coverage (Part D). This creates a single plan, card, and company managing nearly all your healthcare needs, from doctor visits to pharmacy pickups. The appeal often extends to wellness benefits, too, with many plans offering popular perks like free gym memberships. This all-in-one convenience is a key reason for enrollment, but it comes with rules, particularly regarding which providers you can use.
Can You Keep Your Doctor? Understanding HMO vs. PPO Networks

While the extra benefits are appealing, Medicare Advantage plans work within specific rules, the most important of which involves your choice of doctors and hospitals. Each plan has a provider network—the group of doctors, specialists, and hospitals that have agreed to accept its payment terms. The first question you should ask is whether your trusted doctors are “in-network” for any plan you consider.
Many plans are HMOs, or Health Maintenance Organizations. With an HMO, you generally must use providers within the plan’s network to be covered. You’ll also typically choose a primary care physician who coordinates your care and provides a referral before you can see a specialist. The trade-off for these rules is often lower out-of-pocket costs.
A more flexible option is a PPO, or Preferred Provider Organization. With a PPO, you save the most money by staying in-network, but you have the freedom to see an “out-of-network” provider if you’re willing to pay a higher share of the cost. PPOs usually don’t require a referral to see a specialist, giving you more direct control over your healthcare.
Before enrolling, always confirm your doctors are in-network by checking the plan’s official provider directory online or by calling the insurance company. This step is crucial for avoiding surprise bills.
The True Cost: How to Plan for Expenses with an Advantage Plan
A $0 monthly premium for a Medicare Advantage plan doesn’t mean the plan is free. You still pay your monthly Medicare Part B premium to the government. If your income is above certain thresholds, an extra amount called IRMAA may increase your Part B—and sometimes Part D—premiums; factor this into your budget as you compare options. Instead of a high monthly plan fee, you pay for services as you use them through cost-sharing.
This “pay-as-you-go” system works primarily through copays—a fixed fee for a specific service, like a $15 copay for a doctor visit or a $40 copay for a specialist. While the upfront monthly cost can be low, your total spending depends on how much healthcare you need. These small, predictable costs can add up if you require frequent medical attention.
A crucial financial safety net is the out-of-pocket maximum. Every Medicare Advantage plan has a yearly limit on what you will pay for covered medical services. Once your costs reach this maximum, the plan pays 100% for the rest of the year. This feature is essential for limiting financial risk and providing peace of mind.
What Are the Downsides? The Trade-Offs to Consider
The financial predictability of an Advantage plan comes with rules, and the most significant one involves where you can get care. These plans operate within a defined service area, meaning your coverage is tied to a local network of providers. This can be a major disadvantage for anyone who travels frequently or lives in different states part-time, as Original Medicare allows you to see any doctor who accepts Medicare anywhere in the U.S.
Another hurdle you may encounter is prior authorization. This is a process where your doctor must get the plan’s approval before you can receive certain procedures, tests, or expensive medications. While plans use this to manage costs, it can sometimes cause delays in care and be a source of frustration.
Ultimately, the choice is between the go-anywhere flexibility of Original Medicare and the structured benefits of a Part C plan. The right decision depends entirely on your health needs, budget, and lifestyle.
Your Timeline: When and How to Choose a Medicare Plan
Timing is everything, as Medicare enrollment is limited to specific windows set by the government.
For most people, there are three key opportunities to enroll in or change a Medicare Advantage plan:
- Initial Enrollment Period (IEP): A seven-month window around your 65th birthday when you first become eligible.
- Annual Enrollment Period (AEP): From October 15 to December 7 each year, when anyone with Medicare can join, switch, or drop a plan.
- Special Enrollment Period (SEP): A window triggered by specific life events, like moving to a new service area or losing other health coverage.
To start comparing plans, visit the official source: Medicare.gov. Their free, unbiased Plan Finder tool lets you see every plan available in your zip code. You can enter your prescription drugs and preferred doctors to see exactly how each plan would work for you, including special plans for those with chronic conditions. Use it to compare Medicare Advantage plans alongside other options so your healthcare planning stays focused on your needs.
For Chronic Conditions: A Quick Look at Special Needs Plans (SNPs)
Managing a long-term health issue like diabetes or heart disease requires specialized care. Special Needs Plans (SNPs) are Medicare Advantage plans built for people with specific health situations. They offer a focused approach by bundling benefits and services that directly address your diagnosis.
A plan designed for someone with diabetes might offer lower copays for insulin, include extra coverage for foot care, and provide access to nutritionists. The network of doctors is often built around specialists in that field. Because these plans are so targeted, you must have a qualifying diagnosis to enroll. If you do, an SNP could offer more coordinated and affordable care.
Your Next Steps: A Simple Checklist to Find Your Best Path
You now understand the core decision: the à la carte freedom of Original Medicare versus the bundled structure of a Medicare Advantage plan. There is no single “best” plan—only the one that’s best for you.
Your 3-Step Action Plan:
- List Your Must-Haves: Identify your essential doctors, hospitals, and prescription drugs.
- Choose Your Path: Decide if Original Medicare’s freedom or an Advantage plan’s structure fits you better.
- Use the Tool: Go to Medicare.gov to compare specific plans available in your area.
You have the knowledge to turn confusion into confidence. You are no longer a passive recipient of advertising but an empowered shopper equipped to find a plan that serves your health and budget.
Want help choosing the Medicare Advantage plan that actually fits your doctors, prescriptions, and budget?
Schedule a free, no-obligation consultation, and we’ll help you compare plan types (HMO vs. PPO), confirm provider networks, estimate total yearly costs (not just premiums), and map out the right enrollment window.